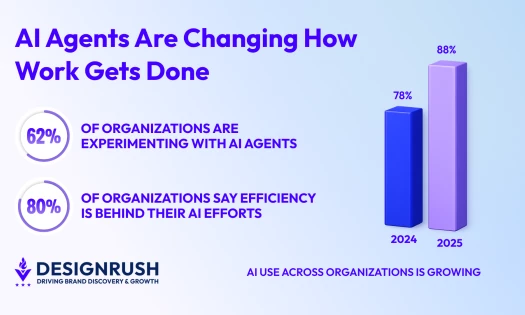
Healthcare Development Key Findings:
- Off-the-shelf tools can't keep up with modern virtual care expectations around personalization, UX, and HIPAA compliance.
- Custom web apps align with clinical workflows, support long-term scalability, and offer built-in security from day one.
- Design, data usability, and deep collaboration are critical to creating digital healthcare tools that improve outcomes.
Is poor virtual care quietly bleeding patients from your business? If so, you could be losing out on roughly 25% more revenue.
One in four patients would opt to switch healthcare providers just to access better virtual care, according to a 2024 study by Deloitte.
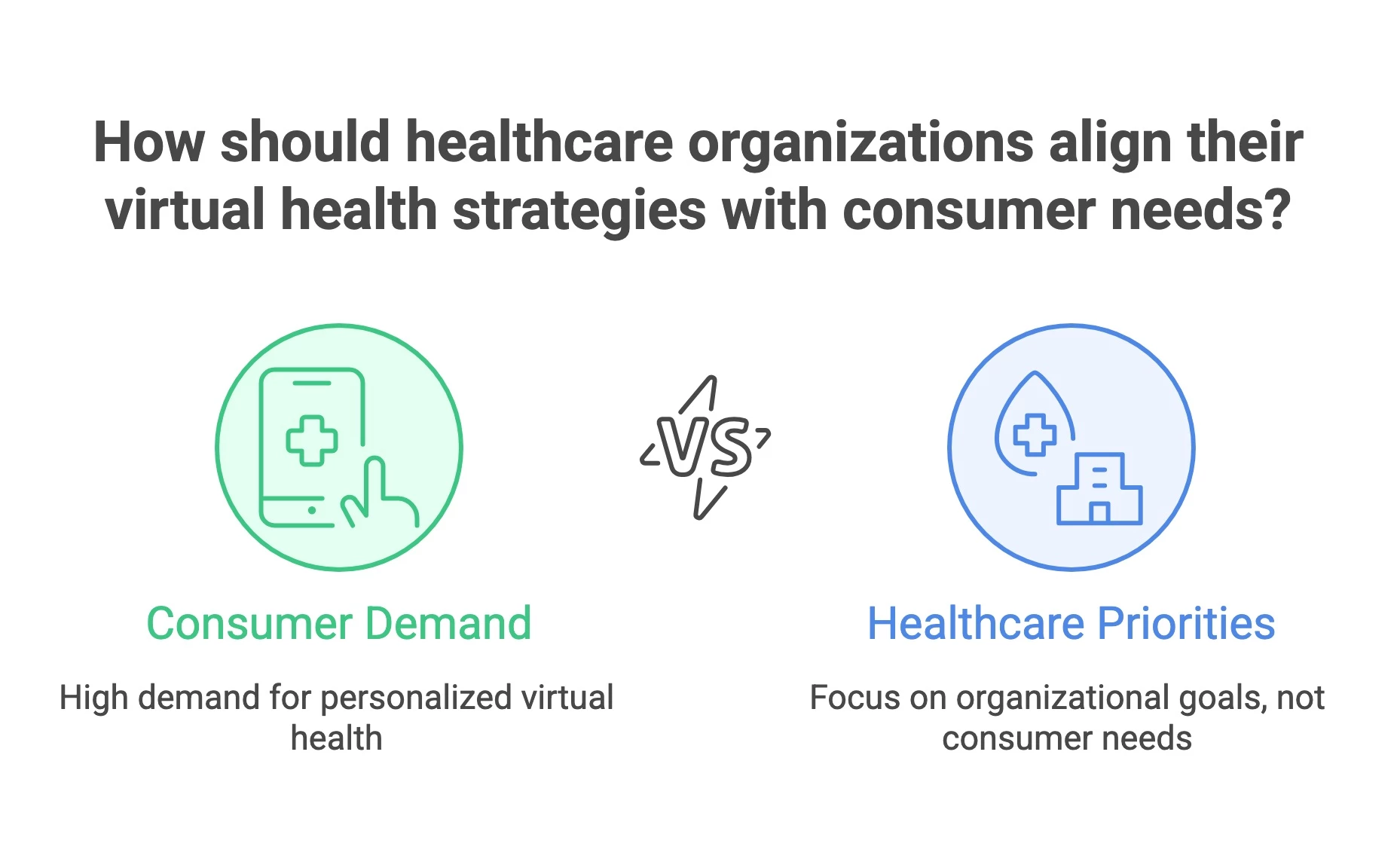
Yet despite rising demand, the use of virtual health services has remained flat since 2022, with some health systems even scaling back or discontinuing their digital offerings altogether.
This disconnect reveals a deeper issue: healthcare providers are still relying on off-the-shelf software that wasn’t built to meet today’s virtual care demands.
These legacy systems can’t keep up with expectations for personalized, accessible, and compliant experiences — the kind of expectations consumers now take for granted in banking, retail, and entertainment.
Editor’s Note: This is a sponsored article created in partnership with Shakuro.
In response, healthcare organizations are turning to custom web applications that give them more control over UX, HIPAA compliance, and long-term scalability.
Development teams like Shakuro say this shift isn’t just about modernizing outdated systems.
It’s about creating digital tools that are secure, interoperable, and aligned with both patient needs and clinical realities.
Here’s why more and more healthcare providers are shifting towards custom web apps to run their practices more efficiently.
1. To Stop Relying on One-Size-Fits-All Software
Out-of-the-box solutions are built to serve the broadest possible user base, which means they rarely meet the specific needs of a single organization — let alone the expectations of modern patients.
Common issues include:
- Rigid workflows: Most platforms force providers to adapt to predefined user flows, making it hard to reflect unique clinical processes or specialties.
- Limited customization: Branding, patient communication, and interface design are often generic, which can hurt trust and usability.
- Patchwork compliance: Many tools offer HIPAA compliance as an add-on or through third-party services, introducing risk instead of reducing it.
- Scalability challenges: As patient volumes increase or new services (like teletherapy or chronic care management) are added, many systems struggle to keep up.
Shakuro notes that these limitations often lead to clunky workarounds, siloed tools, and friction between administrative, technical, and clinical teams.
The result? A fragmented patient experience and rising maintenance costs.
That’s why more healthcare organizations are turning to custom web apps.
These purpose-built tools align with clinical workflows, scale with demand, and meet security and compliance needs from the ground up.
2. To Design Tech Around Care, Not the Other Way Around
Custom-built platforms give healthcare providers control over how digital experiences are designed, delivered, and secured, without relying on workarounds or third-party plugins.
Here’s how they solve for today’s most urgent needs:
- Built-in HIPAA compliance: Security isn’t bolted on after the fact. Custom apps are designed with HIPAA, HITECH, and local data protection laws in mind from the start, ensuring everything from access control to audit trails is integrated at the architecture level.
- Tailored workflows for care teams: Whether it’s streamlining patient intake, triaging by symptoms, or syncing with EHR systems, custom apps reflect your actual day-to-day.
- Scalability without the bloat: As demand grows, custom systems can evolve in lockstep. The codebase is yours to adapt.
- Consumer-grade UX for patients: Today’s patients expect more than a secure portal. Custom apps can offer the frictionless, intuitive interfaces people are used to from banking, eCommerce, and streaming apps, making it easier to engage with care.
View this post on Instagram
“Compliance isn’t just a checkbox — it’s a design principle. Building for HIPAA from day one means thinking through user permissions, audit logs, data access, and even UI elements that reduce the risk of human error,” said Kostya Stepanov, founder and CEO at Shakuro.
3. To Build Around Clinical Workflows, Not the Other Way Around
Off-the-shelf healthcare tools often force clinicians and administrators to adjust their routines to fit rigid system requirements.
This misalignment can introduce unnecessary complexity, slow down care delivery, and reduce the effectiveness of digital interventions.
On the other hand, custom web applications can be designed around the actual workflows and pain points of specific clinical environments.
For example:
- Celéri Health brought together medical practices, device manufacturers, and pharmaceutical companies into a single data loop. Its custom-built platform facilitated seamless information sharing between all stakeholders, enhancing both service delivery and decision-making.
- Alfie, a precision medication platform, focused on personalizing treatment using patient profile data. The UX was designed to support long-term engagement and help clinicians interpret research-backed recommendations at a glance.
When solutions are tailored to how providers actually work, the technology becomes a natural extension of their care, not an obstacle.
4. To Make Healthcare Data Actionable by Design
In healthcare, collecting data is only part of the equation.
The real challenge lies in making that data usable, transforming it into insights that inform clinical decisions, improve patient outcomes, and streamline workflows.
Design plays a critical role here. When dashboards and data visualizations are thoughtfully structured, they make complex information easier to interpret.
That might mean highlighting key patient metrics for faster triage, or organizing operational data in ways that help administrators identify bottlenecks and inefficiencies.
Visual comparisons over time, simplified charts, and intuitive UI elements can reinforce user understanding and support behavior change.
For example, apps that help patients track progress toward health goals are more effective when they allow users to easily see trends and correlations in their behavior or treatment.
In short: data is most powerful when it’s actionable, and that begins with a design that prioritizes clarity, relevance, and real-time feedback.
5. To Collaborate Beyond the Surface to Solve Root Problems
Too often, digital healthcare tools are built to meet surface-level requirements, satisfying a feature list rather than addressing the underlying challenges patients and providers face.
To drive real change, teams must go deeper.
This means moving past cosmetic updates and engaging in meaningful discovery work:
- identifying systemic pain points
- understanding clinical and patient journeys, and
- uncovering opportunities for workflow improvements or behavior change
View this post on Instagram
In practice, that could involve rethinking the structure of a professional practice dashboard so it fits naturally into a clinician’s daily routine.
It could also mean redesigning a patient-facing app to foster long-term engagement instead of one-time use.
Solving healthcare problems at this level demands a process that values co-creation, deep research, and continuous iteration.
“Healthcare isn’t a single-user journey. To build tools that actually work, we collaborate with everyone — from physicians to schedulers to patients — because their workflows are interconnected,” said Stepanov.
Design for Long-Term Use, Not Just Launch
Success in healthcare software isn’t defined at launch.
It’s measured by how well a product holds up over time.
That’s why long-term usability must be baked into the design from the start. Interfaces should guide users intuitively, support habit formation, and adapt to shifting demands without friction.
Companies like Shakuro emphasize that lasting adoption depends on continuous iteration.
Creating tools that people actually want to use — again and again — requires a commitment to usability, flexibility, and empathy at every stage of the product lifecycle.