Key Takeaways:
- 83% of healthcare executives say their infrastructure is too weak to support AI adoption.
- Successful AI adoption in healthcare depends on fitting technology into clinical workflows, not forcing clinicians to change how they work.
- Successful digital transformation requires practical integration, avoiding tech for tech’s sake, and measuring results that matter to both clinicians and patients.
AI adoption in healthcare isn’t moving as fast as it could. About 83% of executives say their infrastructure is too weak to support it, while two-thirds have admitted that it’s become a major roadblock, according to EY.
But tech isn’t the only problem. The biggest issue is building digital tools for healthcare systems without an understanding of day-to-day patient care.
In our interview, Alexander Podgornyy, Managing Director at IT Medical, explains why so many healthtech systems fall short and what leaders should do instead to ensure their AI solutions scale.
Who Is Alexander Podgornyy?
Alexander is the founder and Managing Director of IT Medical, an award-winning software company helping healthcare providers use digital tools more effectively. With more than a decade of product engineering experience and a strong background in healthcare IT, he leads a team that combines clinical insight with modern technology to build secure, scalable, and user-friendly platforms. Under his leadership, IT Medical has become a go-to partner for hospitals, clinics, and healthcare startups around the world.
Editor's Note: This is a sponsored article created in partnership with IT Medical.
Far too often, digital solutions are designed from the top down instead of being built around real-world care. That’s why Alexander believes in staying close to the real problems healthcare teams face every day.
“We never start with the tech. We start with the workflow, the pain points, the inefficiencies,” he explains.
Why? Because that’s where most solutions go wrong. They force clinicians to change how they work, layering complexity onto already strained systems. In other words, tools that tick boxes but get abandoned because they don’t work.
Alexander’s approach? Fit the solution into the workflow, not the other way around. That mindset is what has helped IT Medical scale quickly without losing trust.
Why Digital Transformation Stalls Despite Good Intentions
According to Alexander, traditional systems aren’t built to handle AI’s demands. That’s why digital transformation and AI adoption have been so slow for many healthcare organizations.
You typically need the right compute power, data architecture, and governance frameworks before you can see AI’s full potential, he says.
“To make real progress, healthcare leaders must treat AI adoption as a long-term journey, one that’s grounded in trust, planned for scale, and built with a clear-eyed understanding of what it takes to deliver clinical value.”
Without that mindset, AI in healthcare remains stuck in pilots and promises. IT Medical has even published a guide to help healthcare IT leaders avoid common mistakes.
-content-large-webp.webp)
Simply adding a digital tool (like a patient portal or chatbot) also won’t automatically improve patient experience.
The deeper issues — time-starved clinicians, fragmented communication, and the complexity of navigating care across multiple providers — can’t be addressed with a simple tech-bandaid.
On top of that, patients want information in a way that’s personal, timely, and easy to understand. A static tool or a generic interface won’t help if patients have to deal with health literacy gaps or anxiety around asking follow-up questions.
Instead, Alexander recommends AI-powered assistants because they deliver personalized, real-time support, while clinicians are freed up to focus on the more complex, human side of care.
A Real-World Win: Transforming GI Care with AI
The proof is in the results. IT Medical built an AI-powered GI testing and reporting system for a gastroenterology clinic that was dealing with long backlogs and poor patient communication.
It faced two main challenges:
- The clinic was buried in test backlogs and had no simple way to keep patients informed
- It needed a one-stop digital setup for at-home GI tests, with clear instructions, consent forms, reminders, and symptom tracking
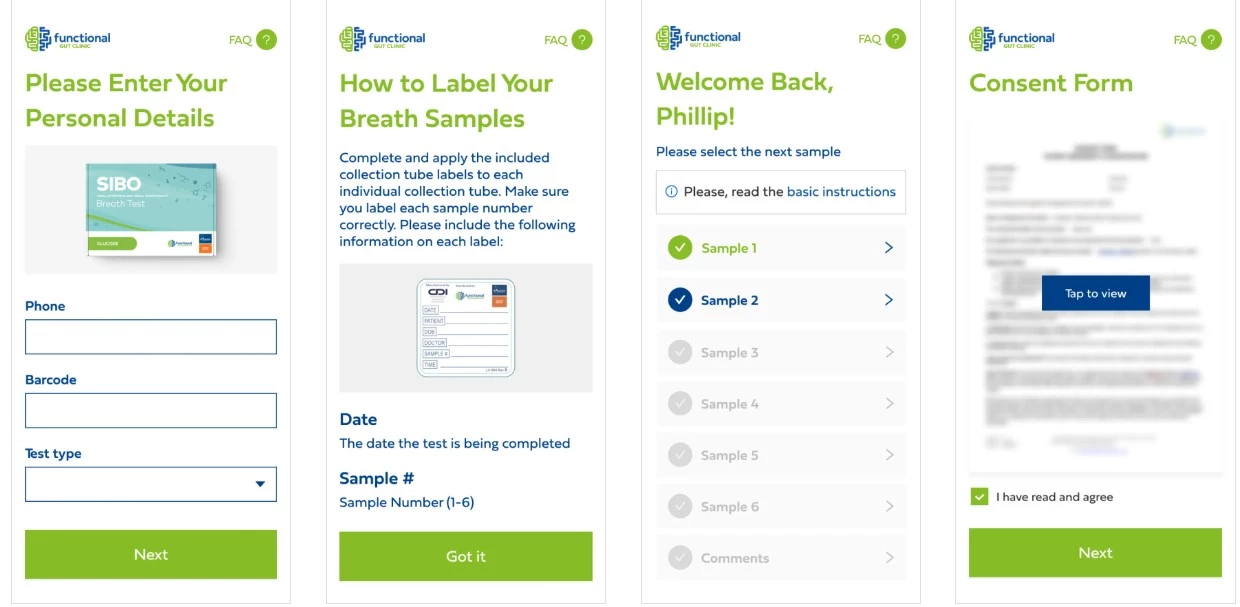
So, IT Medical built a custom system that did the heavy lifting: automating GI test results, sending personalized follow-ups to patients, and giving doctors clear, easy-to-read summaries.
The impact was clear and immediate:
- 75% Reduction in Report Generation Time: Cut report time from 20 minutes to 5, reducing staff workload and improving patient capacity
- 85% Report Automation Coverage: Automated most reports with only minor clinical edits, improving workflow and data accuracy
- 17% Increase in Test Validity: Improved test accuracy with clear instructions and reminders. Over 25% of patients completed tests online

Faster reporting was just the start. The system also helped the clinic spot patterns and gaps they couldn’t see before.
“Digital tools like AI assistants and patient portals can analyze large volumes of data, from symptom patterns to appointment adherence, to reveal hidden care gaps, inefficiencies, or behavioral trends that traditional methods often miss,” Alexander points out.
But knowing what metrics to track is the key to understanding the effectiveness of your new solutions:
- For patients, things like hospital readmissions or how often they visit the doctor show whether care is improving.
- For hospital staff, tracking time spent on paperwork, billing, and data entry reveals how much the tools ease their workload.
- For executives, financial metrics that measure return on investment will help justify the spend on technology.
The right metrics provide a clear picture of whether digital investments are working or just adding noise. Without them, healthcare leaders are flying blind.
Scaling Globally Without Losing Focus
For Alexander, it’s important to stay close to the clinical frontlines. He recommends that founders regularly stay in touch with nurses, doctors, and admins — the people who use their product every day.
“Their feedback is gold. Every market is a bit different, but the core needs are the same: make their jobs easier, not harder,” he says.
Make their jobs easier, keep things simple, be flexible, and never assume you’ve got it right without listening first, he adds.
Scaling matters, but it won’t fix any problems if leadership is disconnected from the frontline.
Digital transformation stalls not because of technology, but because solutions often ignore real clinical challenges.
Alexander says success starts with three things:
- Focusing on real workflows
- Getting users involved from the get-go
- Tracking the right metrics
The AI-powered GI care system is a clear example of how targeted digital tools can reduce workload and improve patient outcomes.
Focus on practical integration, avoid tech for tech’s sake, and measure results that matter to both clinicians and patients.
That’s the real work behind digital transformation.