Key Takeaways:
- Over 70 companies developing AI imaging tools for oncology have raised $6 billion, with 70% backed by venture capital.
- Hospitals looking to integrate AI into imaging systems should focus on phased implementation, data management, and user-centric adoption, among other strategies.
- AI delivers real value when it fits clinical workflows, supports staff, and improves diagnostics without adding complexity.
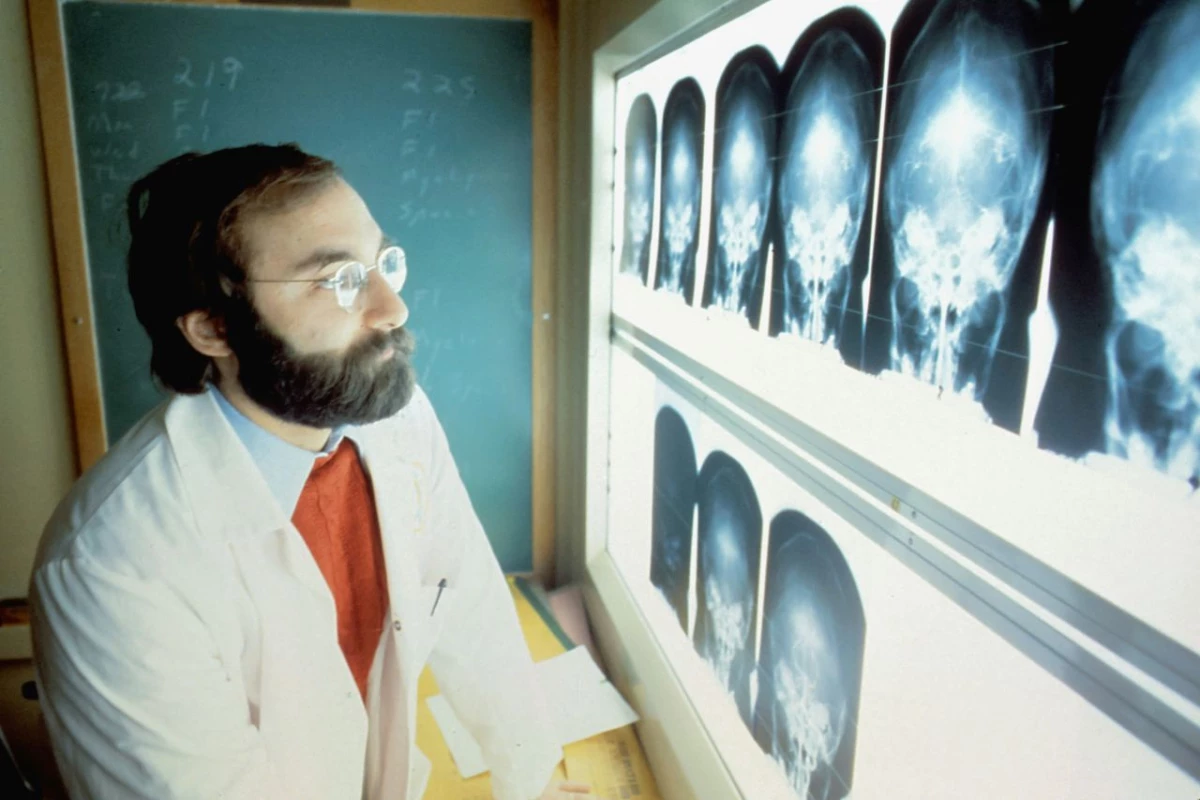
AI-driven solutions are transforming oncology, with over 70 companies working on innovative software and $6 billion in investments. According to Research and Markets, 70% of these were backed by venture capital.
But success goes beyond just the technology.
The real challenge is integrating AI imaging into outdated hospital systems without disruption. This requires a strategic, step-by-step approach to ensure smooth adoption and maximum impact.
There are five key strategies to make this work:
- Phased Implementation
- Interoperability Focus
- Robust Data Management
- User-Centric Adoption
- Continuous Monitoring and Optimization
If done right, AI can improve diagnostics, efficiency, and patient care, according to Clynt Taylor, GM of Health Tech and Life Science at Kanda Software.
Editor's Note: This is a sponsored article created in partnership with Kanda Software.
Modernize Imaging Without Breaking Systems
The full-service product development firm broke this five-step process down as follows:
1. Phased Implementation:
- Start with Pilot Projects: Test AI imaging in specific departments or for simpler use cases, like analyzing routine X-rays in one clinic, before expanding to more complex areas.
- Gradual Rollout: Introduce AI in phases to give staff time to adapt and IT teams the chance to tackle integration challenges.
2. Focus on Interoperability:
- API-First Approach: Choose AI solutions with strong APIs for easy integration into existing healthcare software systems like PACS and EHRs, reducing the need for major changes to legacy infrastructure.
- Adhere to Industry Standards: Opt for AI platforms that comply with healthcare standards like DICOM and HL7 to ensure smooth data exchange across systems
- Data Gateways and Bridges: Use data gateways or bridge solutions to connect older systems with new AI platforms

3. Robust Data Management:
- Data Standardization: Set protocols for cleaning and standardizing data to ensure AI algorithms get consistent, high-quality information from legacy systems
- Secure Data Pipelines: Build secure, reliable pipelines for transferring imaging data to AI platforms, ensuring privacy and compliance with regulations like HIPAA
- Cloud-Based Solutions: Use cloud-based AI platforms for easier scalability and integration with legacy systems, avoiding the need for major infrastructure upgrades
4. User-Centric Adoption Strategies:
- Early Stakeholder Engagement: Involve radiologists, technicians, IT staff, and administrators early to address concerns and gather input
- Comprehensive Training: Offer detailed training on new AI workflows, emphasizing integration with current routines and the benefits, like better accuracy and less workload
- Super User Program: Train key individuals in radiology and IT to lead the way with the new tech and offer peer support
- Clear Communication: Keep communication open about the AI rollout, timelines, and expected benefits to reduce anxiety and resistance
5. Continuous Monitoring and Optimization:
- Performance Monitoring: Set up systems to track the performance of AI imaging tools and their integration with existing systems
- Feedback Mechanisms: Create channels for users to share feedback on AI usability and its impact on workflows
- Iterative Improvement: Use performance data and feedback to refine the integration and optimize AI algorithms for better accuracy and efficiency
By breaking AI adoption into manageable steps, Kanda Software offers healthcare teams a realistic way to bring powerful imaging tools into everyday use without overwhelming staff or disrupting the systems they rely on.
“The integration of AI in medical imaging holds significant promise for improving diagnostic accuracy, increasing efficiency, and ultimately enhancing patient care. However, careful planning and execution are crucial, especially when working with established hospital systems,” said Taylor.
According to Taylor, AI algorithms can assist radiologists and healthcare professionals in several ways, including:
- Detection: Identifying potential abnormalities or areas of interest in images (e.g., detecting tumors, fractures, or hemorrhages).
- Diagnosis: Providing insights that can aid in the diagnosis of diseases and conditions.
- Quantification: Measuring the size, volume, or other characteristics of anatomical structures or lesions.
- Workflow Optimization: Streamlining image analysis workflows, prioritizing urgent cases, and reducing reporting turnaround times.
- Computer-Aided Detection (CADe) and Computer-Aided Diagnosis (CADx): Acting as a "second pair of eyes" for radiologists, CADe systems highlight suspicious areas, while CADx systems may suggest possible diagnoses.
AI imaging only delivers value when it fits the realities of clinical practice.
For decision-makers, that means investing in solutions that support staff, work with existing systems, and improve care without adding complexity.
The payoff isn’t just efficiency — it’s better decisions, faster diagnoses, and stronger outcomes across the board.